by Beth Noyce, RN, BSJMC, HCS-C, BCHH-C, COQS
CHAP-certified home health & hospice consultant
Process Measures
The outcome measures being considered look at effectiveness of hospice clinical efforts to decrease pain and other symptoms. The process measures paired with them focus on the hospice’s follow up with the patient after moderate or severe symptoms are found during assessment.
Exhibit 6 (below) shows the numerator and denominator for these.
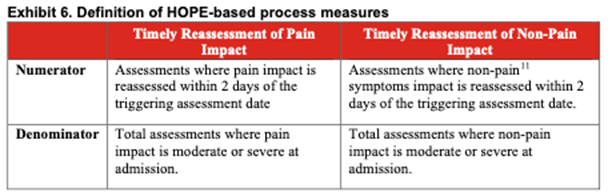
TEP members determined that these two process measures have high face validity. This means the measure items clearly state, or “look like” they will measure what CMS intends them to measure. This allows consumers to see what hospices are assessing and treating. It can also help hospices track how well they are reducing or treating patients’ symptoms.
Katie Wehri, Director of Home Health & Hospice Regulatory Affairs for the National Association for Home Care & Hospice says the face validity of process items is the most important information the HQRP TEP provided to CMS. “Having HOPE items and subsequent measures that actually measure what is intended is key to success,” she says.
Exclusions from Process Measures Success
Exclusions from calculating a hospice’s process measures’ success need careful consideration. Here is the list of options of which patients to exclude:
- Patient desired tolerance level for symptoms
- Patient preferences for symptom management
 Neuropathic pain
Neuropathic pain- Actively Dying (death is imminent)
- Other conditions
The report says that reassessing a symptom within two days of identifying that symptom as moderate or severe is fundamental. This is true regardless of the beneficiary’s stated tolerance-level for symptoms. It also said that process measure calculations should include patients with no symptom-management preference. Further, exclusion criteria should be the same for pain and non-pain symptoms.
Neuropathic Pain
The TEP’s recommends including neuropathic pain in the HOPE tool’s pain-reassessment process measure. Including rather than excluding patients suffering neuropathic pain prompts nurses to reassess these patients for changes. The report references research that suggests 40% of hospice patients may experience neuropathic pain. Patients who experience neuropathic pain have more severe and more distressing pain symptoms. [Tofthagen, C., Visovsky, C., Dominic, S., & McMillan, S. (2019). Neuropathic symptoms, physical and emotional well-being, and quality of life at the end of life. Supportive Care in Cancer, 27(9), 3357-3364. doi:10.1007/s00520-018-4627-x]
The TEP agrees that patients with neuropathic pain should be part of the process measure. However, they recommend excluding the same patients from the outcome measure addressing the patient’s pain impact. The report cited TEP discussion that such pain is chronic and not likely to be resolved or decreased within two days when the reassessment captures outcome data.
The TEP broadly agreed that a nurse who assesses a patient who is actively dying (life expectancy of 3 days or fewer based on clinicians’ assessment) as suffering moderate or severe pain should attempt to reassess the patient. Such patientsshould not be excluded.
The panelists agreed that process measures should include patients of all ages. Several TEP members noted that all patients experience pain and non-pain symptoms, and therefore the measures should apply to adults and children alike.
Exclusion Due to Inability to Reassess
When a hospice is unable to reassess a patient for a valid reason process measures should exclude those patients.
Identified exclusion reason were:
- discharge, alive or dead
- visit refusal
- inability to access the patient due to an emergency department or hospitalization event
- the patient traveling outside of the hospice’s service area
- inability of the hospice to contact the patient or caregiver.
However, the report says, “…hospices should be penalized if reassessment is missing or delayed due to hospice staffing or scheduling issues.”
This article is the second in a series about implementation of HOPE. Next week, Beth Noyce shares details from the panel as it discussed potential future process and outcome measure concepts.
# # #
©2024 by The Rowan Report, Peoria, AZ. All rights reserved. This article originally appeared in Healthcare at Home: The Rowan Report. One copy may be printed for personal use: further reproduction by permission only. editor@therowanreport.com


