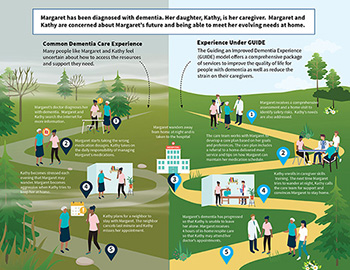
Dr. Oz Nomination Advances to Full Senate
Adminby Tim Rowan, Editor Emeritus
Dr. Oz Nomination Advance to Senate
“Given your close ties to the industry that you would regulate, if you are confirmed, the public would have reason to question your impartiality and commitment to serving the public’s interest.” — Senator Elizabeth Warren, letter to Dr. Mehmet Oz
Reuter’s Ahmed Aboulenein reported on March 12 that “Warren called on Oz to divest from his financial holdings related to industries regulated by the agency and commit to strong ethics safeguards.” Oz, of course, is President Donald Trump’s nominee for CMS Administrator, the agency most important to Home Health and Hospice providers.
Across the aisle, Missouri Senator Josh Hawley peppered Oz with questions about his position on transgender therapy. “You previously praised trans surgeries for minors and supported the use of puberty blockers for children. You discussed transgender therapy on your TV program and hosted transgender children.”
Hawley also questioned Dr Oz’s previous comments on abortion, adding: “I hope he’s changed his views to match President Trump! We need the Trump agenda at CMS.”
It goes without saying that a nominee who encounters challenges from the left and the right is facing an uphill battle toward Senate confirmation, especially when nominees this year can only afford to lose three votes from the majority party. What exactly has Dr. Oz said or done over his long career that may put his nomination in jeopardy?
Pulling Back the Curtain
Becker’s Hospital Review summarized Oz’s history as well as his answers to questions during his three-hour Senate hearing on March 14.
“The former TV personality answered questions about potential Medicaid cuts, the focus of the House’s February budget instruction that the Energy and Commerce Committee cut $880 billion over 10 years. Medicare and Medicaid are the largest programs under the committee’s oversight. (A March 5 Congressional Budget Office report said the only way to reach the $880 billion saving goal over the next decade, without raising taxes, would be through Medicaid or CHIP cuts.)”
While Dr. Oz did not directly respond to questions or reveal his stance regarding Medicaid cuts, he did have a prepared non-answer for the Senators. “I commit to doing whatever I can, working tirelessly to ensure that CMS provides Americans with superb care. Especially Americans who are most vulnerable. Our young, our disabled and our elderly.”

On March 25, the Senate Finance Committee voted to advance Oz’s nomination to the full Senate. The panel voted 14 to 13, along party lines.
Vision Statement
Prior to facing the challenging questions thrown at him from both sides of the aisle, Dr. Oz used his opening statement to outline a vision focused largely on modernizing CMS’s systems; addressing waste, fraud and abuse; and incentivizing Americans to make healthier lifestyle choices.
In the past, Oz had endorsed privatizing Medicare through a change that would essentially result in something that might be called “Medicare Advantage for All.” In his Senate hearing answers, Oz pivoted to the opposite argument. He cited problems of overpayments to Medicare Advantage plans, the need to limit prior authorizations, and emphasized the need to halt the practice of “upcoding” where providers or plans bill for treating patients as sicker than they actually are.
In 2010, Dr Oz hosted a 15-minute segment on his show called “Transgender Kids: Too Young to Decide?” in which he spoke to transgender children, their parents and a doctor who provided gender-affirming care.
Outlook
Considering the slim Republican majority in the Senate, Ox can afford to lose only three Republican votes in his bid to become the next CMS administrator.
# # #

Tim Rowan is a 30-year home care technology consultant who co-founded and served as Editor and principal writer of this publication for 25 years. He continues to occasionally contribute news and analysis articles under The Rowan Report’s new ownership. He also continues to work part-time as a Home Care recruiting and retention consultant. More information: RowanResources.com
Tim@RowanResources.com
©2024 by The Rowan Report, Peoria, AZ. All rights reserved. This article originally appeared in Healthcare at Home: The Rowan Report. One copy may be printed for personal use: further reproduction by permission only. editor@therowanreport.com