Subsidies Undecided
Medicaidby Kristin Rowan, Editor
Subsidies Undecided
Senate cannot agree
The record-breaking government shutdown centered around one issue: extending the COVID-era Affordable Care Act supplemental subsidies. The subsidies were an additional discount for Americans within a certain income bracket. They helped make healthcare insurance through the ACA marketplace more affordable during and after COVID. The subsidies have been extended multiple times and expire at the end of the year. Senate Republicans are not willing to extend them again. Senate Democrats won’t vote in favor of any health care proposal that doesn’t include them.
Time is Running Out
Not only do the subsidies expire at the end of the year, but anyone enrolling in a marketplace plan has to apply by December 15th, leaving precious few days to find a way forward. Senate Democrats proposed a straight three-year extension of the subsidies, which failed. Senate Republicans proposed using the subsidy money to contribute to HSAs for bronze or “catastrophic” plans. That proposal also failed.
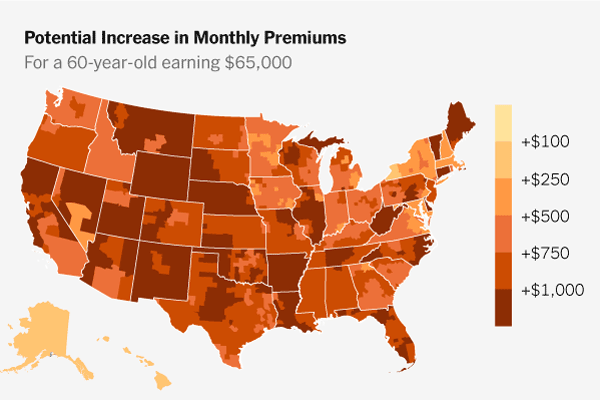
A hybrid compromise is in the works. Details have not been released but it will likely include income caps and eligibility restrictions on the subsidies as well as some HSA flexibility. Without an extension on the subsidies, premiums are expected to increase an average of 26% in 2026, although some analyses suggest premiums could go up by 73-90%.
Another Shutdown?
The 43-day shutdown that ended in November did not finalize the 2026 budget. It merely passed enough appropriations to temporarily fund some departments through January 30, 2026 and a few essential departments for longer. If the Senate and House cannot agree on the subsidy issue, we face another shutdown in February. Every shutdown impacts Medicare & Medicaid payments, approvals, and renewals.
Experts indicate nearly 50% of people buying marketplace plans are ages 50-64. Most, if not all of them, are looking at lower cost (and lower benefit) plans or dropping insurance altogether in 2026. If insurance costs remain high, this group of

people will enter Medicare with poorer health, which will cost the Medicare program and tax payers more in the long run. It will cause a vicious circle of higher Medicare costs, leading to higher taxes, lower subsidies, higher premiums, fewer people being covered, and finally higher Medicare costs again.
This is an ongoing story and The Rowan Report will continue to bring you the latest news on the subsidies and the impending expiration of the temporary government funding as we head into 2026.
# # #


Kristin Rowan has been working at The Rowan Report since 2008. She is the owner and Editor-in-chief of The Rowan Report, the industry’s most trusted source for care at home news, and speaker on Artificial Intelligence and Lone Worker Safety and state and national conferences.
She also runs Girard Marketing Group, a multi-faceted boutique marketing firm specializing in content creation, social media management, and event marketing. Connect with Kristin directly kristin@girardmarketinggroup.com or www.girardmarketinggroup.com
©2025 by The Rowan Report, Peoria, AZ. All rights reserved. This article originally appeared in The Rowan Report. One copy may be printed for personal use: further reproduction by permission only. editor@therowanreport.com