Home Care Patient Dies in Care: Aide Arrested
by Kristin Rowan, Editor
Elderly Patient Needs 24-hour Care
In Polk County, FL, an 86-year old man, identified only as Mr. Anderson, was hopsitalized and diagnosed with congestive heart failure. In addition to receiving care from Good Shepherd Hospice, his family hired round-the-clock care through Assisting Hands. The home health aides were caring for Mr. Anderson in 12-hour shifts.
Night Shift
Beatrice Taylor arrived for her night shift at 9 p.m. She noted that Mr. Anderson and his wife were already in bed, but not sleeping. Shortly after the day aide left, Taylor fell asleep on the couch in the living room of the patient’s home. Company policy states she was responsible for the patient’s care and should not have been sleeping.
An Avoidable Tragedy
Taylor was awakened by a “thump” coming from the bedroom. She entered the bedroom to investigate and found Mr. Anderson lying on his side, on the floor, with his head wedged between the nightstand and the bed. Taylor told investigators that she tried to help him back into the bed. He told her not to touch him, so she left him there and went back to sleep on the couch. She did not call 911, as was the policy of Assisting Hands in the event of an emergency. Nor did she call her agency or anyone else to assist.
Four Hours Later
Taylor woke up somewhere between 3:45 a.m. and 4:53 a.m. that morning. At some point, she called her parents and had a 36 minute conversation. During that conversation, she decided to check on the patient and found him still on the floor, but now unresponsive. It was her parents who suggested she call 911.
Contrary to both her parents’ urging and her employer’s policy, Taylor still did not call 911. Instead, she called Assisting Hands and left a message through the company portal. Taylor finally called 911 at 5:37 a.m., more than four and a half hours after Mr. Anderson fell.
The implanted pacemaker found during autopsy showed that Mr. Anderson was still allive at 1:oo a.m. when Taylor initially found him. The autopsy also concluded that he would have survived if Taylor had called 911 right away. His official cause of death was positional asphyxia with pre-existing health conditions listed as contributory causes.

Not actual image from story
Company Policies Broken
- If a patient falls, home aides are required to seek help which may entail calling 9-1-1. Home aides must notify the company as soon as the patient is safe
- Home aides are not permitted to sleep during their assigned shift unless it is a “live in” shift
- Home aides are required to submit care notes using the company portal throughout their shift to ensure assigned services are being followed appropriately.
The 911 call that Taylor placed at 5:37 a.m. should have been placed at 1:00 a.m.
Assisting Hands confirmed to detectives that this was not a “live in” shift
No information was provided as to whether Taylor submitted care notes during the shift.
Arrested Development
Taylor worked for Assisting Hands for eight months, but did not show up for her shift following the incident with Mr. Anderson. Assisting Hands has since terminated her employment. She was a licensed home health aide, but does not have a medical license, nor is she a nurse.
Taylor was arrested by detectives and made several statements about her innocence. She insisted she had done nothing wrong saying she, “didn’t kill that man.” A paramedic who responded to her 911 call overheard Taylor on the phone say, “he was old anyway so what does it matter.” Taylor remains in custody at the Polk County Jail and is being held without bond.
Polk County Sheriff
“The complete disregard for Mr. Anderson’s life by the person who was employed by his family is completely outrageous, and egregious. I believe someone who was not even being paid to look after this elderly man would have immediately dialed 9-1-1 under these circumstances. Her behavior and attitude are simply deplorable. Mr. Anderson’s family members are in our prayers.”
Risk Fall
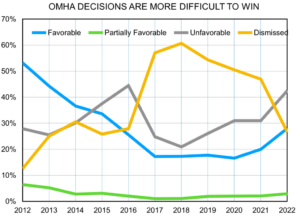
In 2021, more than 38,000 older adults died from falls. This is the leading cause of injury death for adults aged 65 and older. The death rate increased 41% between 2012 and 2021. You can read more about the risk of falling and what one company is doing to help prevent falls in our accompanying article this week, an interview with Dr. Ann Wells of InnovAge.
# # #


Kristin Rowan has been working at Healthcare at Home: The Rowan Report since 2008. She has a master’s degree in business administration and marketing and runs Girard Marketing Group, a multi-faceted boutique marketing firm specializing in event planning, sales, and marketing strategy. She has recently taken on the role of Editor of The Rowan Report and will add her voice to current Home Care topics as well as marketing tips for home care agencies. Connect with Kristin directly kristin@girardmarketinggroup.com or www.girardmarketinggroup.com
©2024 by The Rowan Report, Peoria, AZ. All rights reserved. This article originally appeared in Healthcare at Home: The Rowan Report. One copy may be printed for personal use: further reproduction by permission only. editor@therowanreport.com