The $100,000 Visa
by Kristin Rowan, Editor
The $100,000 Visa
What Care at Home Needs to Know
Highly skilled, highly trained, and highly in-demand professionals fill roles that very few are qualified to hold. These roles are usually in math, engineering, technology, medical science. They can also be in healthcare, trade jobs like plumbers and welders, and professional fields like financial managers and market research analysts.
Due to the specialized training and education, extensive experience, and other unique qualifications required for these positions, the number of people qualified to fill them is much lower than the number of positions to fill. The U.S. has relied on the H-1B visa, a type of permission for highly skilled professions to work temporarily in the U.S. in these specialty jobs. The H-1B visa starts at three years, but can be extended to six.
H-B Visa Availability & Distribution
Very few of these visas are available. Standard H-1B visas are capped at 65,000 per year. There are an additional 20,000 H-1B visas available only to persons who have earned a master’s degree or doctorate from a U.S. school.
Currently more than 70% of H-1B visa holders have citizenship in India. The largest petitioners for H-1B visas are tech and retail giants Amazon, Microsoft, Meta, Apple, Google, Cognizant Technology Solutions, JPMorgan Chase, and Walmart.
Executive Order
On September 21, the fee to petition for a new H-1B visa increased from $2,000-5,000, depending on the size of the employer, to $100,000. This change was implemented by proclamation. The administration has since clarified that the fee will apply to new petitions, not those already in process and that it is a one-time fee.
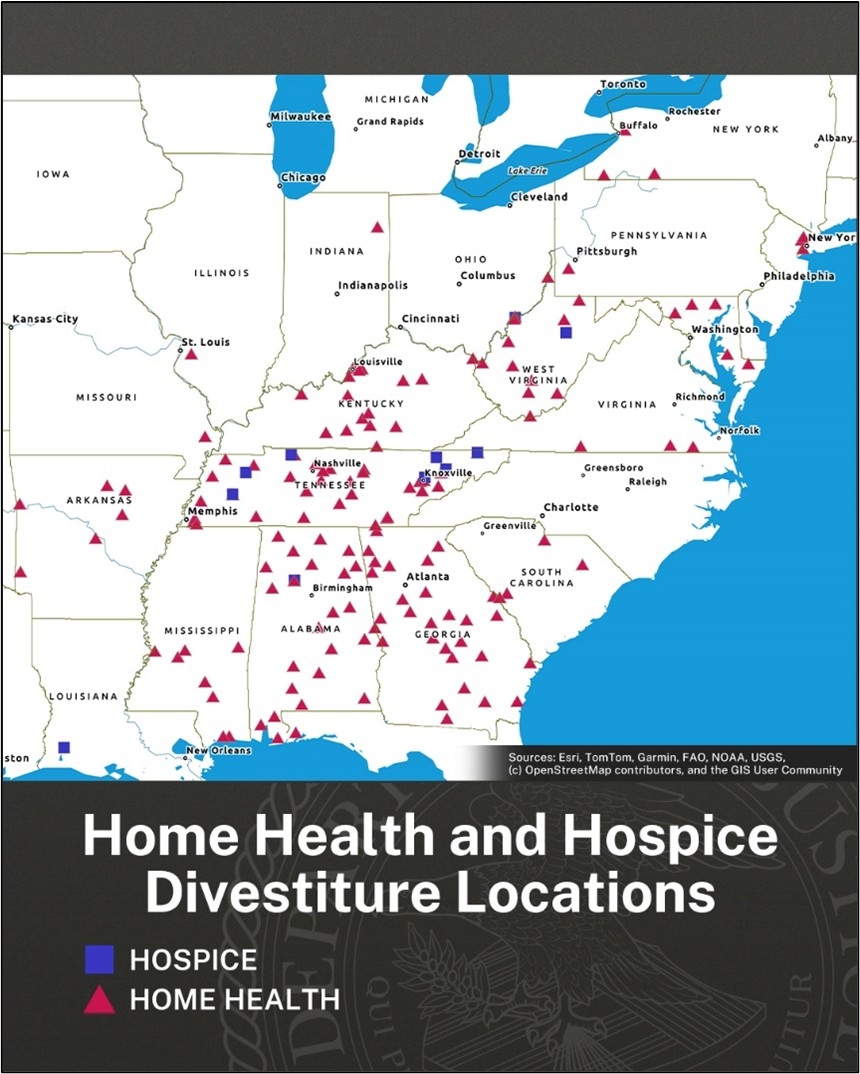
Impact on Care at Home
According to Becker’s Hospital Review, healthcare uses the H-1B visa often to sponsor medical residents and physicians. Overall, immigrant workers account for 27% of physicians and surgeons, 22% of nursing assistants, and 16% of RNs nationwide. Included in the proclamation is an exemption clause. This allows the $100,000 visa fee to be waived if the Secretary of Homeland Security decides, on an individual basis, for specific companies, that the hiring is in the national interest. It is unclear whether that exemption will extend to health care workers.
According to Ellis Porter, immigration attorneys, standard nursing positions do not qualify for H-1B visas because they are not considered “specialty occupations.” RNs in the U.S. must have a two-year associate’s degree, not the required bachelor’s degree for the H-1B visa. Ellis Porter says even if you have a bachelor’s degree, that alone does not qualify an RN for an H-1B visa. Nurse Managers, Nurse Practitioners, Certified Registered Nurse Anesthetists, Certified Nurse Midwives, and Clinical Nurse Specialists qualify as “specialty occupations” under the H-1B visa regulations.
If healthcare workers are not exempt from the new fee, some nurse positions will be effected. This could increase the workforce shortage for nurses outside the care at home industry, driving care at home nurses into hospitals, medical centers, doctor’s offices, and SNFs, which could, in turn, exacerbate the workforce shortage for care at home. However, until there is clarity on the exemption, this is not a definite.
$100,000 Visa Overturned
Immigration attorneys are already preparing lawsuits to challendge the proclamation. They are calling it excessive, unlawful, and equal to a ban on immigrant workers. Some critics argue the proclamation bypassed established rulemaking procedures. Others say there are provisions to charge visa fees to cover expenses, but no legal precedent to charge exorbitant fees. Legal experts call the proclamation vague and arbitrary, leaving it open for misinterpretation, and therefore is likely to be overturned.
This is an ongoing story that requires additional clarification and explanation. The White House has promised an FAQ page soon. We will continue to follow this story as it develops.
# # #


Kristin Rowan has been working at The Rowan Report since 2008. She is the owner and Editor-in-chief of The Rowan Report, the industry’s most trusted source for care at home news, and speaker on Artificial Intelligence and Lone Worker Safety and state and national conferences.
She also runs Girard Marketing Group, a multi-faceted boutique marketing firm specializing in content creation, social media management, and event marketing. Connect with Kristin directly kristin@girardmarketinggroup.com or www.girardmarketinggroup.com
©2025 by The Rowan Report, Peoria, AZ. All rights reserved. This article originally appeared in The Rowan Report. One copy may be printed for personal use: further reproduction by permission only. editor@therowanreport.com