Home Health in a Post-Chevron World
by Elizabeth E. Hogue, Esq.
The "Wicked Witch" Chevron is Gone
On June 28, 2024, the U.S. Supreme Court overturned a decision of the Court in 1984 often referred to as “Chevron.” The Chevron case said that Courts must defer to administrative actions that are reasonable interpretations of ambiguous statutory language.
In Loper Bright Enterprises v. Raimondo, however, the U.S. Supreme Court abandoned the decision in Chevron and said that:
-
- The “deference that Chevron requires of courts reviewing agency action cannot be squared with” the Administrative Procedure Act (APA). The APA “specified that courts, not agencies, will decide ‘all relevant questions of law’ arising on review of agency action…even those involving ambiguous laws – and set aside any such action inconsistent with the law as they interpret it.”
- The framers of the U.S. Constitution envisioned that the final “interpretation of the laws” would be “the proper and peculiar province of the courts.”
- The views of the executive branch should inform the judgment of the judiciary, not supersede it.
- “Chevron’s presumption is misguided because agencies have no special competence in resolving statutory ambiguities. Courts do.”
What Does it Mean for Providers?
The short answer is that we don’t know yet. It is unclear how the new standards of the Loper Bright decision will be applied and affect health care providers. The Supreme Court said that the recent Court decision does not call past cases into question that were based on Chevron, but existing regulations are not insulated from challenges. It is likely that several providers will “swing for the fences” for favorable rulings based on Loper Bright!
One possible “candidate” for disruption is the reliance of administrative law judges (ALJs) on Chapter 8 of the Medicare Program Integrity Manual. This section offers an overview of use of inferential statistics and statistical sampling to estimate overpayments in Medicare audits. Chapter 8 of the Manual is only nine pages long. ALJs routinely use this section of the Manual to hamper providers’ ability to mount a compelling defense that challenges auditors’ methods using widely accepted standards within the statistical community. Challenges to this practice based on Loper Bright may prevent ALJs from reliance on these sections of the Manual.
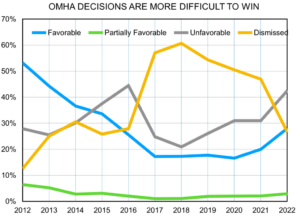
Another possible target is the use of sub-statutory and even sub-regulatory guidance from the Centers for Medicare and Medicaid Services (CMS) and the Medicare Administrative Contractors (MACs) by fraud and abuse enforcers to make determinations about illegal conduct, especially under the False Claims Act (FCA). Defendants arguably now have a better chance to challenge the basis of claims of illegal conduct in light of Loper Bright.
The story of Loper Bright has not been written by any means. Surely providers should use this significant change in the law to their benefit whenever possible.
# # #


Elizabeth Hogue is an attorney in private practice with extensive experience in health care. She represents clients across the U.S., including professional associations, managed care providers, hospitals, long-term care facilities, home health agencies, durable medical equipment companies, and hospices.
©2024 by The Rowan Report, Peoria, AZ. All rights reserved. This article originally appeared in Healthcare at Home: The Rowan Report. One copy may be printed for personal use: further reproduction by permission only. editor@therowanreport.com
©2024 Elizabeth E. Hogue, Esq. All rights reserved.
No portion of this material may be reproduced in any form without the advance written permission of the author.