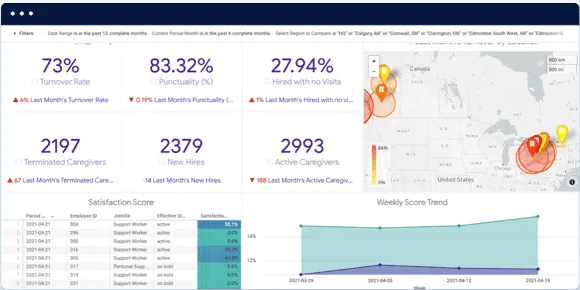
Ava is an enterprise AI platform helping healthcare providers streamline administrative busywork so that they can get back to care. In an industry where employee engagement and retention are crucial yet increasingly challenging to maintain, Ava provides an effective AI-driven solution that’s beneficial for clients, caregivers, and providers. Integrating seamlessly with Electronic Health Records (EHRs), Ava offers an engaging experience for caregivers and clinicians while providing administrators with a robust suite of tools for business intelligence, employee management, and gamified incentives. For more information, visit joinava.com.
Department of Labor Changes Exemption and Overtime Thresholds
by Tim Rowan, Editor Emeritus
Overtime and exemption thresholds impact employers trying to balance cost-effective policies with employee fairness. As such, they keep a close eye on rules they must follow that come down from the U.S. Department of Labor. When those rules change, remaining compliant requires a company HR leader to adapt those policies. One of those times is at hand.
Exemption and Overtime Thresholds for Hourly and Salaried Earners
Effective last week, July 1, the annual salary threshold for overtime exemption increased from $35,568 to $43,888. The DoL’s final rule does not stop there but sets another increase on January 1, 2025, to $58,656 per year or $1,128 per week. Salaries below those thresholds cannot be declared “exempt,” meaning they must be paid overtime rates for hours worked over eight per day and forty per week.
Executive Salaries also Affected
In addition to overtime and exemption thresholds, the new rule increases the highly compensated employee threshold twice as well. On July 1, the annual salary threshold increased from $107,432 to $132,964. That annual threshold will increase again on January 1 to $151,164.
Going forward, the DOL will increase all thresholds every three years starting July 1, 2027, relying on up-to-date wage data.
We learned these DoL rule details from Angelo Spinola, Executive Director and lead home care attorney with Polsinelli, a national law firm.

Angelo Spinola Comments
“Home care providers that have been making adjustments to comply with the July 1 deadline may have heard about a recent case out of Texas blocking the July 1 increases. While the Texas court did use a partial injunction blocking the July 1 increase, it only applies to Texas government employees. It does not affect any private employers.”
He recommended that all home health and home care employers continue to make changes as planned to comply with the July 1 increases. Spinola stated that his statements are for informational purposes only and are not intended to be legal advice. His comments quoted here should not be relied upon or used without consulting a lawyer to consider your specific circumstances, possible changes to applicable laws, rules and regulations and other legal issues.
Spinola Concludes
“There are still challenges pending that could affect the January 1, 2025 increases, however, those decisions are not expected for several months, and it is too soon to predict whether that deadline will be affected. We will continue to monitor these cases and provide any updates that may have an effect on the home care industry.”
Angelo Spinola can be reached via email at onlinesolutions@polsinelli.com.
NAHC Comments on Exemption and Overtime Thresholds
“The long-awaited U.S. Department of Labor rule regulating minimum salaries levels to qualify for exemption to the Fair Labor Standards Act was issued today. We strongly advise the home care community to gain a comprehensive understanding of the rule and institute steps for timely compliance. While the changes may have limited impact on most home care companies, noncompliance comes with serious penalties.” – NAHC President Bill Dombi
# # #

Tim Rowan is a 30-year home care technology consultant who co-founded and served as Editor and principal writer of this publication for 25 years. He continues to occasionally contribute news and analysis articles under The Rowan Report’s new ownership. He also continues to work part-time as a Home Care recruiting and retention consultant. More information: RowanResources.com
Tim@RowanResources.com
©2024 by The Rowan Report, Peoria, AZ. All rights reserved. This article originally appeared in Healthcare at Home: The Rowan Report.homecaretechreport.com One copy may be printed for personal use: further reproduction by permission only. editor@homecaretechreport.com