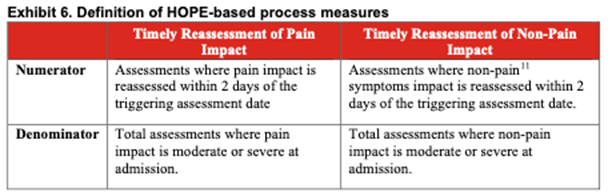
New Resources for Home Health Value-Based Purchasing Model
Clinicalby Kristin Rowan, Editor
The Home Health Value-Based Purchasing (HHVBP) Model began in 2016 as part of the Home Health Prospective Payment System (HH PPS) final rule. The original model aimed to:
- Incentivize better quality and more efficient care
- Study potential quality and efficiency measures
- Enhance the public reporting process
HHVBP Model Outcomes
The original model had an average 4.6 percent improvement in Total Performance Scores (TPS). The model also saved Medicare $141 million annually, on average. There were no adverse risks with these savings.
Additionally, the model reduced the number of unplanned hospitalizations and stays at Skilled Nursing Facilities (SNF). This provided additional savings from lower inpatient and SNF spending.
HHVBP Expansion Model
The HHVBP model expanded in 2022. The model includes HHAs in all 50 states, D.C., and the U.S. territories. The model adjusts Medicare payments from the fee-for-service (FFS) model. Quality measures in a Performance Year impact adjustments in the Payment Year. These adjustments range from -5% to 5% and are based on quality measures relative to peer performance. HHA peers are pre-assigned cohorts with HHAs of similar size.
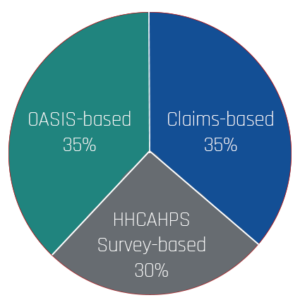
The expanded HHVBP model uses data from the Home Health Quality Reporting Program (HH QRP), Medicare claims, and HHCAHPS surveys. The expanded model does not require any additional data at this time.
Additional information on the quality measures, cohorts, guides, and recordings from CMS can be found here.
We will continue to follow this story and provide updates on the new expanded model as they come in.
# # #


Kristin Rowan has been working at Healthcare at Home: The Rowan Report since 2008. She has a master’s degree in business administration and marketing and runs Girard Marketing Group, a multi-faceted boutique marketing firm specializing in event planning, sales, and marketing strategy. She has recently taken on the role of Editor of The Rowan Report and will add her voice to current Home Care topics as well as marketing tips for home care agencies. Connect with Kristin directly kristin@girardmarketinggroup.com or www.girardmarketinggroup.com
©2024 by The Rowan Report, Peoria, AZ. All rights reserved. This article originally appeared in Healthcare at Home: The Rowan Report. One copy may be printed for personal use: further reproduction by permission only. editor@therowanreport.com










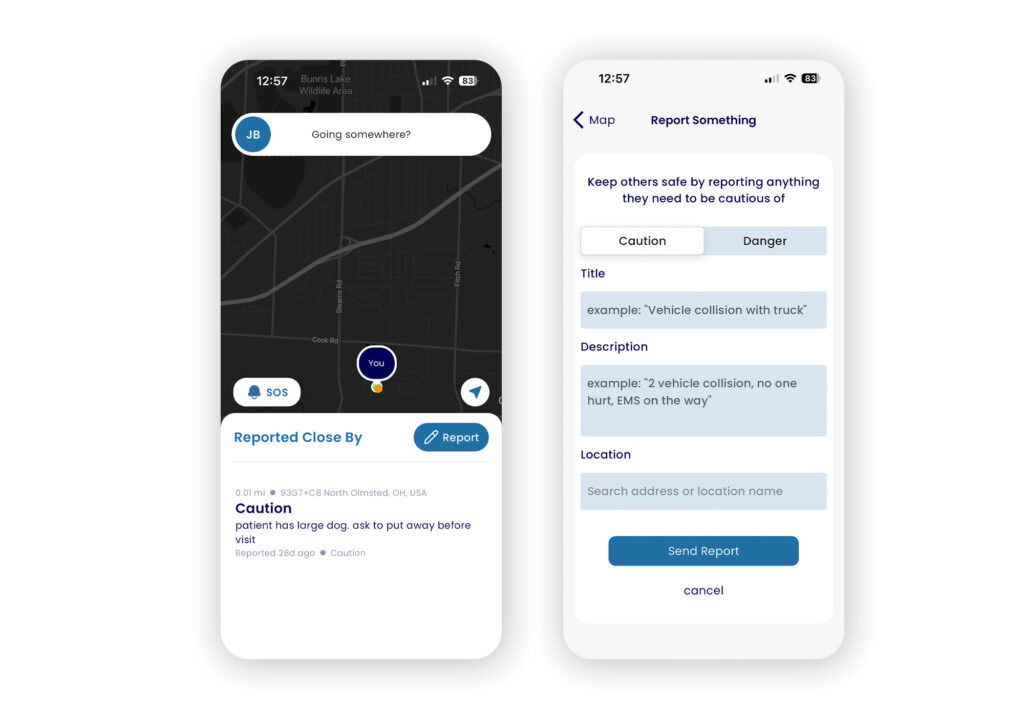










 Joyce Grayson murder during a home health visit, leadership in Connecticut aimed to safeguard home health and home health aide workers and collect risk assessment data on the same.
Joyce Grayson murder during a home health visit, leadership in Connecticut aimed to safeguard home health and home health aide workers and collect risk assessment data on the same.
 “We realized that caregivers get little to no guidance within the health care system,” said Shahed Alam, a co-founder of Noora Health. Many patients do not know why they are receiving care. Doctors and nurses tend repeat the same information to patient after patient.
“We realized that caregivers get little to no guidance within the health care system,” said Shahed Alam, a co-founder of Noora Health. Many patients do not know why they are receiving care. Doctors and nurses tend repeat the same information to patient after patient.



 Between 2014 and 2023, at least 34% of fraud convictions in some years were based on private duty home care services. In some years, this percentage was as high as 48%.
Between 2014 and 2023, at least 34% of fraud convictions in some years were based on private duty home care services. In some years, this percentage was as high as 48%.